Clinical Improvement/Innovation
31 - Surgical Case Delay Notification – Emergency Case Priority
Location: Hall E

Rachel L. Cipolli, RN, BSN, MSN, CCRN, CPHQ (she/her/hers)
Patient Care Director
New York Presbyterian
Tappan, New York, United States
Primary Poster Author(s)
Disclosure(s):
Rachel L. LaPoma, RN, BSN, MSN, CCRN, CPHQ: No financial relationships to disclose
Description:
1. Team Description This multidisciplinary team includes perioperative nurses, surgeons, transplant coordinators, anesthesiologists, and OR leadership at a high-acuity academic medical center. They manage over 23,000 surgeries annually, including complex cases like trauma and organ transplants. Each member contributes specialized clinical and operational expertise to ensure safe, efficient, and patient-centered care in a dynamic environment.
2. Preparation and Planning The team identified inefficiencies in handling unplanned or urgent procedures, often caused by overreliance on verbal communication (e.g., phone calls), leading to delays and miscommunication. To address this, they launched a Lean and human-centered design initiative. Lean healthcare principles were applied to map communication flows, identify handoff points, and document inefficiencies. Engaging frontline staff and clinicians ensured the solution was practical and aligned with clinical needs.
3. Assessment A thorough evaluation revealed that the absence of a centralized, transparent, and asynchronous communication system caused scheduling conflicts, duplicated efforts, and care delays. The assessment included: Auditing surgical records to quantify unplanned procedures. Monitoring communication patterns for delays and escalation. Conducting staff interviews to identify workflow bottlenecks. These issues compromised patient safety, operational flow, and staff well-being.
4. Implementation To improve coordination, the team implemented digital tools tailored to their clinical environment, including: A centralized case-tracking dashboard accessible to perioperative staff, anesthesiology, and surgical teams. A HIPAA-compliant secure messaging platform enabling asynchronous communication, reducing phone interruptions. These tools were integrated with the EHR to enhance visibility of case updates, room turnover, and prioritization. Staff received training, and usage metrics were tracked to support adoption and continuous improvement.
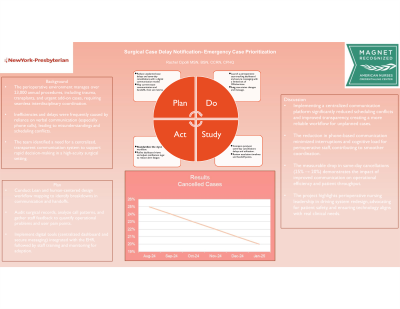
5. Outcomes Post-implementation, the team observed: A drop in same-day cancellations of unplanned cases from 25% to 20%, improving efficiency. Increased staff satisfaction, with surveys citing reduced stress and improved workflow transparency. Better OR utilization and scheduling, enhancing resource allocation and patient throughput.
6. Implications for Perioperative Nursing This initiative highlights the critical role of perioperative nurses in coordinating surgical care and driving operational improvements. By leading communication enhancements, nurses directly influence patient safety, care quality, and team performance. Their involvement in technology adoption and workflow redesign reinforces the value of nursing leadership in delivering safe, efficient, and patient-centered surgical care."
