
Joseph Masong, BSN-RN (he/him/his)
Perioperative Clinical Manager
New York Presbyterian
Nanuet, New York, United States
Primary Poster Author(s)
Disclosure(s):
Joseph Masong, BSN-RN: No financial relationships to disclose
Description: Description of Team:
Operating Room RN, Surgical Team, Scheduling Team, Project Manager
Assessment:
At a large academic medical center, the neurosurgery department continues to expand to meet the growing demand for specialized care. To accommodate this increate in patient volume, the operating room (OR) team recognized the need to evaluate and optimize key efficiency metrics such as first case on time starts (FCOTS) and turn around time (TAT). Improving these metrics was essential for streamlining surgical throughout, minimizing delays, and creating capacity for add-on cases.
Preparation & Planning:
A multidisciplinary team was formed including surgeons, clinical nurses, certified surgical technologists (CST), anesthesia providers, Central Sterile Processing Department (CSPD) staff, and project manager. The team began by reviewing baseline efficiency metrics, developing current-state process maps, and conducting interviews with all frontline team members to gain a comprehensive understanding of existing workflows and pain points. A formal kickoff meeting was held to present the findings and launch the process improvement initiative.
Implementation:
Four focused workgroups were established: Scheduling, CSPD, Intraop, PACU. Each workgroup tasked with addressing specific areas of opportunity. These workgroups met weekly, and then reported out monthly at the larger group meeting.
In the CSPD workgroup an emergency case cart was created to support urgent add on cases, new surgical clips were trialed, additional trays were ordered based on utilization.
The PACU workgroup designed and implemented a new workflow for managing light-sensitive medication.
To improve scheduling accuracy, a standardized set of booking codes were developed and tutorials provided to booking team.
Within the intraoperative workgroup several initiatives were launched including the implementation digital whiteboard to assist with daily flow, creation of position carts, established monthly check-ins with team leader and residents, and root cause analysis of any delay that exceeded goal.
Outcome:
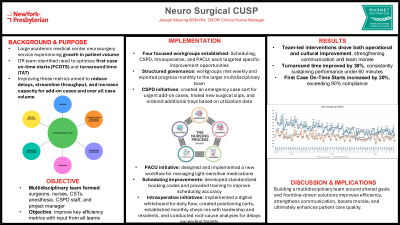
Through focused, team-led interventions, the impact extended beyond efficiency metrics to a meaningful cultural shift that strengthened communication and boosted team morale. Turnaround times improved by 30%, consistently achieving and sustaining the goal of under 60 minutes. First Case On-Time Starts (FCOTS) increased by 20%, surpassing 90% compliance. While scheduling accuracy has shown modest improvement, it remains the most significant area of opportunity. Notably, the team has reported enhanced collaboration and communication, reflecting a positive shift in the overall work environment.
Implication:
Forming a multidisciplinary team, aligning a shared vision and goals, and implementing ideas from frontline staff not only enhances efficiency, it also strengthens communication, improves team morale, and ultimately elevates the quality of care we provide to our patients.
Ezeh, C. E., H John Cooper, Vitale, M. G., Butrico, E., Camera, D., & Lu, K. (2024). The Impact of the Comprehensive Unit-Based Safety Program on the Perioperative Efficiency and Patient Safety of Adult Hip and Knee Arthroplasty Procedures. the Journal of Arthroplasty/the Journal of Arthroplasty. https://doi.org/10.1016/j.arth.2024.03.027
Friedman, D. M. (2004). Improving Team Structure and Communication. Archives of Surgery, 139(11), 1194. https://doi.org/10.1001/archsurg.139.11.1194
